It is estimated that over two million Americans have some type of glaucoma and half of them do not know it. Ninety percent of glaucoma patients have open-angle glaucoma. Although it cannot be cured, it can usually be controlled. Vision loss may be minimized with early treatment. The eye receives its nourishment from a clear fluid that circulates inside the eye.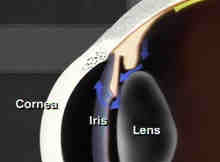
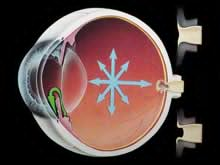
This fluid must be constantly returned to the blood stream through the eye's drainage canal, called the trabecular meshwork. In the case of open-angle glaucoma, something has gone wrong with the drainage canal. When the fluid cannot drain fast enough, pressure inside the eye begins to build.
This excess fluid pressure pushes against the delicate optic nerve that connects the eye to the brain. If the pressure remains too high for too long, irreversible vision loss can occur.
Symptoms of open-angle glaucoma:
- In the early stages, there are no symptoms of blurred vision or pain
- Gradual loss of peripheral vision (the top, sides and bottom areas of vision) that is not perceptible to most people until the disease is in the advanced stages

Normal vision (left) and Loss of peripheral vision due to advanced glaucoma (right)
Who is at risk:
Glaucoma can occur in people of all races at any age. However, the likelihood of developing glaucoma increases if you:
- are African American
- have a family history of glaucoma
- are diabetic
- are very nearsighted
- are over 40 years of age
Diagnosing open-angle glaucoma:
Everyone should be checked for glaucoma at around age 35 and especially at age 40 and over. Those considered to be at higher risk, including those over the age of 60 should have their pressure checked every year or two. Ideally, you should have an eye exam every two years no matter what age you are.
Your doctor will use tonometry to check your eye pressure. After applying numbing drops, the tonometer is gently pressed against the eye and its resistance is measured and recorded.





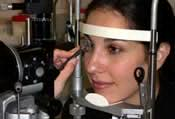
Eye pressure is not directly related to blood pressure. The "normal" pressure ranges from 10 to 21. However, it is important to know that many people with eye pressure in the normal range have glaucoma, and many with pressure above the normal range do not. There are many other factors that determine glaucoma, including:
The Optic Nerve: This is the structure in the eye that suffers damage from eye pressure that is too high for an individual eye to tolerate. An ophthalmoscope can be used to examine the shape and color of your optic nerve. The ophthalmoscope magnifies and lights up the inside of the eye. Cupping or atrophy of the optic nerve will be carefully evaluated. If the optic nerve appears to be cupped or is not a healthy pink color, additional tests will be run. At Karlik Ophthalmology, all patients that are suspicious for glaucoma or diagnosed with glaucoma have the health of their optic nerves documented with digital retinal imaging. Imaging is repeated if any progressive damage to a patient's optic nerve is evident.
Optic Nerve Scanning is performed at Karlik Ophthalmology using a Heidelberg Retinal Tomograph (HRT). This scanning laser measures the nerve tissue present in the optic nerve of each eye. Repeat measurements by the HRT can be obtained to document progressive optic nerve damage before they may be evident on examination. This technology assists the doctors at Karlik Ophthalmology in diagnosing glaucoma at the earliest stages and ensures that each glaucoma patient's disease is being adequately treated.
Perimetry, or visual field testing, is a test that maps the field of vision. Looking straight ahead into a white, bowl-shaped area, you will indicate when you are able to detect lights as they are brought into your field of vision. This map allows your doctor to see any pattern of side or peripheral vision changes caused by the early stages of glaucoma. This is a somewhat tedious test for the patient, but with modern instruments can be done in 15 minutes or less. The results are extremely important in diagnosing and managing glaucoma.
Gonioscopy is used to check whether the angle where the iris meets the cornea is open or closed. This helps your doctor determine if they are dealing with open-angle glaucoma or narrow-angle glaucoma. Narrow angle glaucoma (please refer to the section on this condition) is a fairly uncommon condition. Most people with glaucoma have the open angle variety. Gonioscopy is the procedure that helps determine which type of glaucoma you have. Gonioscopy also helps determine how appropriate laser treatment (SLT) may be in a patient with glaucoma.
Treatments for open-angle glaucoma:
To control glaucoma, treatment has been traditionally started with medication. This typically requires the daily instillation of eye drops for life. With advancements made in laser treatment, initial treatment of open angle glaucoma can now be performed with a laser (SLT) in the office.
Glaucoma medicines come in eye drop form and medications to be taken by mouth. Oral medications (tablets and capsules) are rarely used anymore due to side effects, but are still an option. Drops work by either slowing the production of fluid within the eye or by improving the flow through the drainage meshwork. To be effective, most glaucoma medications must be taken once or twice every day, without fail. Some of these medications have some undesirable side effects, so your doctor will work with you to find a medication that controls your pressure with the least amount of side effects. Medicines should never be stopped without consulting your doctor, and you should notify all of your other doctors about the eye medications you are taking.
Selective Laser Trabeculoplasty (SLT) is an in-office laser procedure designed to open the drainage canal of the eye, resulting in a reduction of the pressure of the eye. Patients can typically drive home after having this laser procedure performed in the offices of Karlik Ophthalmology. Requiring only numbing eye drops, the laser beam is applied to the trabecular meshwork resulting in an improved rate of drainage. When laser surgery is successful, it may reduce or eliminate the need for daily medications. For reasons of convenience, side-effects, and expense, many patients now choose this laser procedure (SLT) over the life-long daily requirement of eyedrops which was once necessary for the treatment of open angle glaucoma. The doctors of Karlik Ophthalmology discuss this option with all patients diagnosed with open angle glaucoma.
Endoscopic CycloPhotocoagulation (ECP) is another type of laser procedure. Instead of treating the drainage canal, it treats the ciliary body. Treating the ciliary body reduces the amount of fluid production thereby reducing the intraocular pressure. ECP is most often performed along with cataract surgery, but can be done on an outpatient basis when in the best interest of the patient. The majority of patients having ECP reduce or eliminate their need to take glaucoma medications.
Filtration surgery is performed when medicines and/or laser surgery are unsuccessful in controlling eye pressure. During this microscopic procedure, a new drainage channel is created to allow fluid to drain from the eye.
Procedures:
 Glaucoma medication comes in many forms  Laser surgery can reduce the need for daily medication  Filtration surgery |